Medical imaging is a vital yet costly component of healthcare
Americans spend nearly 20% of our gross domestic product on healthcare,1 totaling $3.65 Trillion in 2018. One in every ten of those dollars was spent on medical imaging procedures,2 which may not be surprising considering that medical imaging has become one of the most important tools for diagnosing and treating the most devastating health conditions such as cancer, stroke and heart disease. While these benefits are indisputable, studies have shown that up to one-third of all imaging exams is unnecessary,3 meaning that we are potentially wasting in excess of $100 Billion each year. Furthermore, although it is more difficult to quantify, healthcare providers spend an inordinate amount of wasted time tracking down the images that they need to provide efficient care—especially image-intensive specialists in oncology, neurology, orthopedic medicine and cardiology. And finally, although Computed Tomography (CT) imaging is one of the most powerful of these imaging modalities, with 80 million studies being performed per year and saving many lives, the radiation exposure to patients from CT imaging is projected to cause approximately 2% of future cancers according to the FDA.4
Medical image sharing is a critically underserved need
Within this environment, coupled with the continually growing emphasis on value-based care, it is critical that healthcare providers maximize the value of this enormous investment in medical imaging by making images more readily accessible at the point of care. This requires that images from providers across the care community be shared efficiently and effectively. Traditional methods such as shipping or hand-carrying CDs or maintaining spiderwebs of point-to-point VPNs have been shown to be cumbersome, ineffective and costly. Cloud-based, dedicated image sharing networks have therefore grown in popularity in recent years, and while they are clearly a step ahead of previous approaches, they still fall short of the mark when it comes to providing efficient delivery of diagnostic quality images at the point of care in concert with a patient’s full medical record:
- Stand-alone image sharing networks still require numerous manual steps at the requesting/destination as well as the responding/source location. This is not only costly, but it also serves as an unnecessary distraction to care providers from focusing on actual patient care.
- Stand-alone image sharing networks are typically not able to reconcile patient identities and records across locations in a comprehensive way. Therefore, assuring that a patient’s complete relevant imaging history is available in a timely way is at best a “hit-or-miss” proposition.
- Requiring physicians and other care providers to access yet one more “information silo” dedicated to images adds to an already overwhelming burden that they are already struggling with on a daily basis.
eHealth Technologies, in collaboration with many of the leading local, regional and state-wide Health Information Exchanges (HIEs) has recognized this need by including access to diagnostic quality medical images as an integral part of their patient’s longitudinal records. eHealth Connect Image Exchange provides a tightly integrated suite of image sharing workflows that enable faster, more efficient and effective care delivered by healthcare providers who are constituents of an HIE. By leveraging the underlying infrastructure that already exists for sharing other nonimaging records—such as master patient identification systems (MPIs), patient consent management, and record locater services—a much more comprehensive, automated community-wide image sharing solution is now possible.
Stand-alone image sharing networks are helpful but are still costly and inefficient
The diagram below depicts a typical stand-alone image sharing network workflow. In addition to the fees paid for an image sharing cloud service, the 8 steps that are shown may very well consume several days of calendar time and hours of administrative overhead—just to accomplish the “simple” task of accessing external medical images.
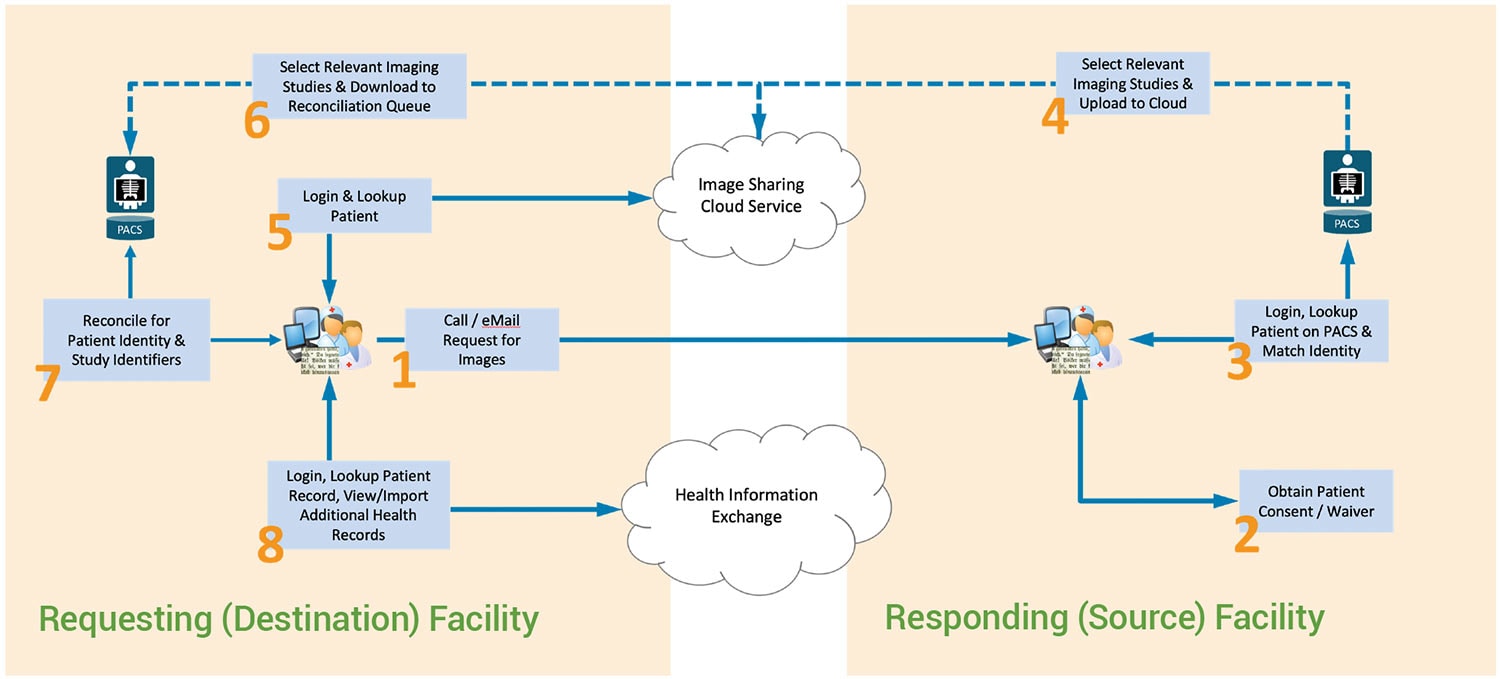
Typical “Stand-Alone” Image Sharing Network Workflow
- A requesting facility identifies a need to view or import an imaging study from an external facility. Once the various external locations where images might reside are identified (often by having to ask the patient), a representative must notify each source facility of their need, often by a phone call or email.
- Source facility personnel may be required to obtain a consent or a waiver from their patients before they can share their images with another facility. This can once again require further phone calls or emails.
- Once consent is obtained, the source facility must match patient identities with their own patient records before images can be shared, often with incomplete or inconsistent demographic data. This not only wastes more time, but it also carries the risk of mismatching patient records, creating the clinical risk of merging records from different patients.
- When the associated patient’s imaging records have been located, the relevant subset of images, as determined by the source facility’s personnel, must be uploaded to an image sharing cloud service.
- Once images have been uploaded, the requesting facility must log in to the image sharing cloud service and look up their patient’s imaging record.
- Relevant images are identified and downloaded into a local image reconciliation queue, awaiting further processing.
- In order to properly merge a patient’s images with those stored on a local PACS, a “reconciliation” process is required to update patient identifiers (MRNs) in the external images’ DICOM headers before a final import.
- External medical images are finally available to radiologists, cardiologists and other image-intensive caregivers at the requesting facility. However, if additional external non-imaging records are needed, they will need to access yet another system such as the Health Information Exchange.
Image-enabled HIEs with eHealth Connect Image Exchange solve the remaining challenges
eHealth Connect Image Exchange, when integrated with an existing HIE, reduces the manual steps from 8 to at most 3, eliminates ALL manual steps at the source facility, and happens in minutes rather than hours or days as depicted below.
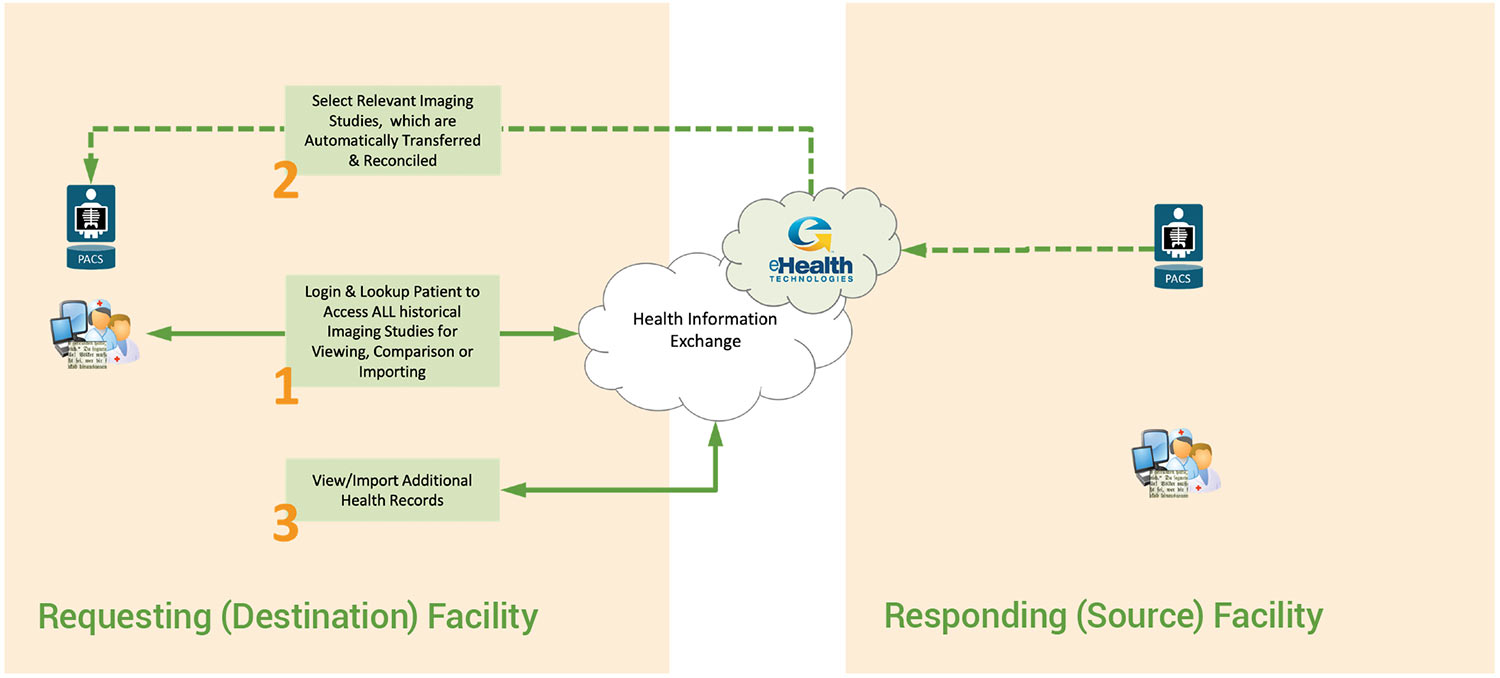
Image-Enabled HIE Workflow using eHealth Connect Image Exchange
- A requesting facility identifies a need to view or import an imaging study from an external facility. Logging in to the Health Information Exchange, which can frequently be done with a single click from an EMR, RIS or PACS, provides care providers with immediate access to ALL historical imaging studies for their patient at ALL connected facilities.
- Selecting the relevant imaging studies can be accomplished with a single click. Images can be viewed directly on the HIE, or imported with reconciliation being performed as a “background” task so that they contain the appropriate patient identifiers before being stored on the destination PACS.
- If non-imaging health records are needed, they are accessible from the same location as images on the HIE.
With an HIE that is image-enabled by eHealth Connect® Image Exchange there is:
- NO need to log in to multiple systems for images and other patient records. The HIE provides a single access point for ALL images and ALL other records from ALL participating facilities.
- NO need to manually reconcile patient identities between locations, as this is a capability that is provided by the HIE.
- NO need to obtain patient consent to share images from the source facility, as this is also a capability provided by the HIE.
- NO need for source facility personnel to locate a patient’s images and push them to the cloud. This is all done automatically behind the scenes.
- NO risk of missing a vital prior image from another facility because someone at the source location failed to locate and upload it. eHealth Connect Image Exchange allows HIE users to be “image aware” making ALL historical images at ALL participating facilities readily accessible.
- CMS.gov 2016-2025 Projections of National Health Expenditures
- Harvey L. Neiman Health Policy Institute brief #1: “Medical Imaging: Is the Growth Boom Over?”
- Consumer Reports.org “The surprising dangers of CT scans and X-rays”
- US Food & Drug Administration: “What are the Radiation Risks from CT?”